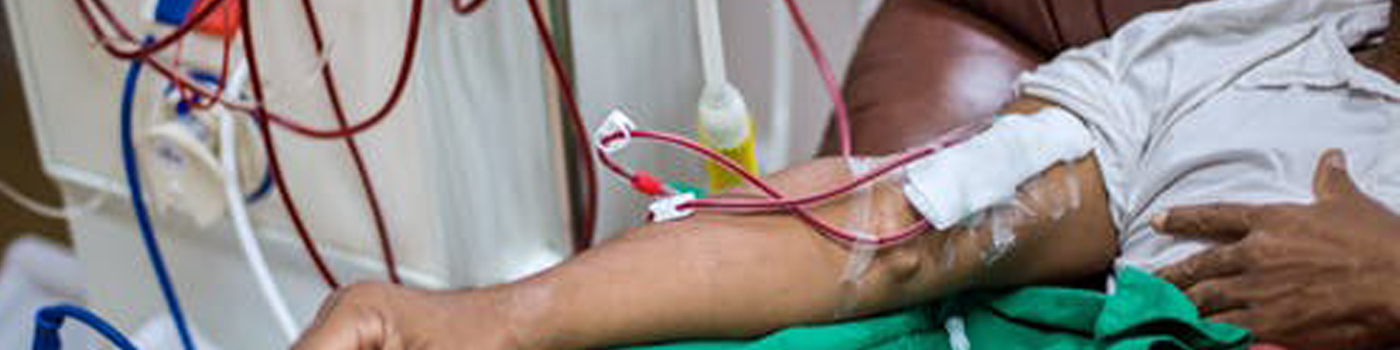
Your Hemodialysis Unit
Waiting Area
Please be patient and make yourself comfortable in the waiting area until you are called for your treatment. In the waiting area, there is information and articles about kidney disease and other topics of interest.
Restrooms
We have restrooms in the unit for patients. Each restroom has a call bell in case you do not feel well or need help. Visitors are to use the public restrooms.
Smoke-free
There is no smoking anywhere in the building or near entrances and exists.
Food and drinks
Patients are encouraged to have a meal prior to treatment; if they are unable to, they are permitted to bring a small snack or meal of their choice to have before or during treatment. However, the Centre will not assume any risk for the patient’s consumption of the meal while receiving treatment and as such will not assist in any way with preparation or consumption of the meal or snack. Some of the potential risks of eating or drinking while having your dialysis treatment include, but are not limited to:
- Lowering of blood pressure and reduction in the circulation of blood flow
- Nausea – possible vomiting and choking
- Urgent need for a bowel movement or even diarrhea, shortening treatment time
- Cramping
The safety of our patients is paramount to us and, as such, we must follow international standards in regard to consumption of meals, which include fluids such as water, juice, etc.
If you have diabetes, remember to bring a snack in case you need one during hemodialysis.




What to bring
Televisions are provided for the entertainment of all patients, but it is suggested that you bring what you may need to make you more comfortable. It is cold in the unit and blankets are not provided. We suggest that you bring a blanket, pillow/neck roll, a book, laptop, music device with ear plugs, etc.
Visitors
Visitors are not allowed in the treatment area and must remain in the waiting area.
Preparing for Hemodialysis Treatments
Clothes
Wear loose, comfortable clothing that allows easy access to your dialysis access site. Wear clothes that can be washed easily, in case blood or other liquids are spilled on your clothes.
Medication
Bring all medicines that you take to your first treatment, including:
- Over-the counter medicines
- Prescribed medicines from all physicians
- Herbal medicines
- Vitamins and supplements
Our medical team checks your medications with you. At every treatment, bring in any new medication you have been prescribed and those you need to take during treatment.
Discuss with your doctor whether your medication or the timing of your medication needs to change on dialysis days.
Always carry a list of your medications in your wallet or purse.
Arriving
Please arrive on time for your scheduled treatment. Coming in earlier does not get you on hemodialysis faster and, as a result, you might have to wait a long time before we can start your treatment at your scheduled time.
Always remain in the waiting area until we come to get you. This keeps the treatment area clear and safer for everyone. When it is your turn, we bring you to your hemodialysis station.
Weighing in
Healthy kidneys control the fluid balance in our bodies, and dialysis does this job when our kidneys stop working. Healthy kidneys work 24 hours every day removing extra fluid and waste products. When kidneys don’t work properly, urine production slows down and sometimes stops completely, so the need to remove the leftover fluid during dialysis becomes very important. Tracking the exact amount of fluid that goes in and comes out of your body isn’t practical, so we use a “goal” or “dry” weight to tell the story of how much extra fluid is left in your body.
You will weigh in BEFORE and AFTER every hemodialysis treatment. When you weigh, remove heavy shoes and any heavy clothing. Write down your weight and give it your nurse. You will have the same scale to use before and after dialysis.
Your doctor decides on your ‘goal’ or ‘dry’ weight. This is the weight that is best for you to reach at the end of each dialysis treatment.
Weighing in before your treatment helps us figure out how much water needs to be removed from your body.
As you start to feel better, you might have a better appetite. We might need to increase your ‘goal weight’. Let your nurse and dietitian know if you think you might be gaining weight.
Did you know?
One kilogram [Kg] of body weight is equal to one litre [L] of body fluid. If you need to lose 2 kilograms, the hemodialysis machine removes 2 litres of body water.
Before your treatment is started:
- Wash your hands with soap for at least 45 seconds. Remember the best way to stop the spread of infection is to wash your hands. If you need to touch your access site after washing your hands, clean your hands with an alcohol hand sanitizer.
- Wash your access site before your treatment. If your access site is in your leg, use the washroom to wash the area.
- Tell us if you have seen any doctors or had to stay in the hospital since your last treatment.
- Tell us if you have had any changes to medications since your last treatment. Remember to bring in any new medications.
- Tell us if you have had any unusual health events since your last treatment. e.g., cramping, fatigue, a fall.
- Tell us if you do not feel well. The nurse will want to complete a detailed check of your health.
- Collect what you need before you settle into your chair.
- We check your heart rate, temperature, and blood pressure (both standing and sitting). Leave the blood pressure cuff on so we can check your blood pressure during your treatment.
Your Hemodialysis Treatment
Before the treatment
It is normal to feel nervous when you first start hemodialysis. Your nurse or technician explains how the hemodialysis machine works. Ask as many questions as you may need to.
If you have a fistula or graft, two needles will be inserted, to begin dialysis. (see section on Vascular Access). One needle takes the blood out of your body and the other returns the cleaned blood to your body. To keep your fistula or graft working properly, we place the needles into different parts of the fistula or graft with each treatment. You should not feel any pain once the needles are in place. Tell your nurse if you do have pain or discomfort during your treatment.
If you have a catheter, we connect you to the machine using the two different ends of your catheter.
Blood is drawn monthly before and after dialysis to ensure your dialysis dose is adequate and to see if changes to your treatment are necessary.
During your treatment
During hemodialysis, only about 1 cup (250 mL) of blood is outside the body at any time. You do not feel the blood going in and out of your body.
There are side effects to hemodialysis that you may experience and should tell us about right away if they occur:
- Cramping
- Headaches
- Feeling dizzy or faint
- Feeling restless
- Sweating or feeling warmer than usual
- Feeling sick to your stomach (nauseated)
- Feeling like you need to move your bowels
- Feeling your heart racing
- Having blurred vision
If you feel anything unusual, let us know right away, so we can help you.
You can help yourself by keeping to your diet and fluid limits between treatments. Going over your limits increases the amount of fluid that must be removed during treatment. Removing a large amount of fluid is one of the things that may make you feel sick.
After your treatment
We check your heart rate and blood pressure (both standing and sitting) and in some cases, your temperature.
Some people get a low blood pressure after the treatment. If you feel faint, dizzy, or lightheaded after your hemodialysis:
- Sit down right away.
- Tell someone that you do not feel well.
- For your safety, we will not let you leave until you are feeling better. If you do not recover right away, we might arrange for you to go to another area for care until you feel better.
When your hemodialysis treatment is finished, your nurse or technician removes the needles. If you have a fistula or graft, apply pressure to the needle sites for at least 10 minutes to stop the bleeding.
To hold pressure over the needle sites:
- Always clean your hands.
- Hold a gauze pad over the needle site using two fingers. Press at the needle spot and just above.
- Hold constant firm pressure for at least 10 minutes.
- We might take out one needle at a time and ask you to hold each site, one at a time.
Your nurse or technician will instruct you on how this is done.
Once the bleeding has stopped:
- Place a clean gauze pad over the needle site and tape in place. NEVER wrap the tape around our arm (or leg). If you do, it can reduce the blood supply to your fistula or graft and possibly stop blood flow.
- Wash your hands.
Before you leave
Weigh yourself again. Remember to wear the same clothing and use the same scale. We want to check that the right amount of water weight was removed. Remove your heavy shoes and any heavy clothing.
Always wash your hands with soap. This helps stop the spread of any germs you might have contacted during the treatment.
In the beginning you may not be feeling well. Arrange to have someone drive you home as you adjust to dialysis treatments. You might get very tired after hemodialysis, so it is safer if someone drives you.
At home – Take it easy
Rest when you get home from dialysis. You might feel quite tired. Many people feel better once they have been on hemodialysis for a few weeks.
Possible Side Effects of Treatment
Some patients may experience side effects during and after treatment, though not often. The nurses and technicians are always available and will be there to assist you. Recognizing the early symptoms can help in early interventions by the staff, should any of these occur.
You can reduce the likelihood of side effects by keeping to your diet and fluid levels between treatments.
Call your Hemodialysis Unit right away if:
- You experience persistent cramping, dizziness, fainting, nausea or blurred vision.
- You can’t feel the “thrill” (a buzzing sensation around the fistula) or if it feels different from usual (fistula or graft).
- There is redness, warmth, pain or swelling in your access arm (fistula or graft) or along your catheter.
- There is any oozing or drainage from your fistula, graft or catheter exit site.
- You have noticeable swelling in your access arm (fistula or graft) or around your catheter, neck or face.
- You are feverish and have any of the above symptoms.
- Part of your catheter outside your skin seems to be getting longer.
- Your catheter is accidentally pulled and there is bleeding around the exit site.